Complex therapies. Simpler payment.
Specialty pharmacies manage high-cost medications, prior authorizations, and patients with more at stake. Tabz handles the payment side of that complexity so your team can focus on the clinical side.

Patients who pay before dispensing
Of those pay within the first hour
Average time to collect patient payments
Average payout window to pharmacies
Average patient satisfaction rating
Specialty pharmacy is high-stakes on both sides. A single uncollected copay on a high-cost therapy can mean thousands of dollars written off. Prior auth delays stall dispensing, patients drop out of therapy, and staff spend hours coordinating between payers, prescribers, and patients by phone. Tabz digitizes the payment and communication layer so work only moves forward when commitments are real.

How Tabz works for specialty pharmacies
Copay collected before high-cost dispensing
Patients pay their portion before a high-cost therapy ships or is dispensed, eliminating write-offs on expensive unclaimed medications.
Prior auth and missing info resolved digitally
When prior auth or patient info is needed, Tabz sends a direct message with a link to complete it. No phone tag, no delays waiting for callbacks.
Adherence support and refill reminders
Automated messages keep specialty patients on their therapy schedule. Refill reminders, shipment updates, and payment requests go out at the right moment without staff intervention.
HSA/FSA and copay assistance supported
Patients pay with HSA/FSA where eligible. Copay assistance programs can be applied at checkout, reducing friction for patients on manufacturer support.
PMS-connected payment workflow
Tabz connects directly to PioneerRx, Liberty, Keycentrix, PK Software, Computer-Rx, and other systems. Prescription and copay data flows into the payment workflow automatically, with no manual re-entry.
HIPAA-ready and Level 1 PCI DSS certified
Built to meet the compliance requirements of specialty pharmacy, including sensitive therapy categories, payer data, and patient privacy obligations.
The unified pharmacy commerce platform.
Tabz connects payment, communication, fulfillment, and reporting into a single operating platform. Each capability runs on the same foundation, so every transaction stays aligned from checkout to reconciliation.

Increase revenue
with higher conversions
Copay amounts, digital wallets, and HSA/FSA card payments integrated directly into prescription workflows. Patients pay by text link or email — whether they're picking up in store or receiving a delivery. Payment collected before the order moves.
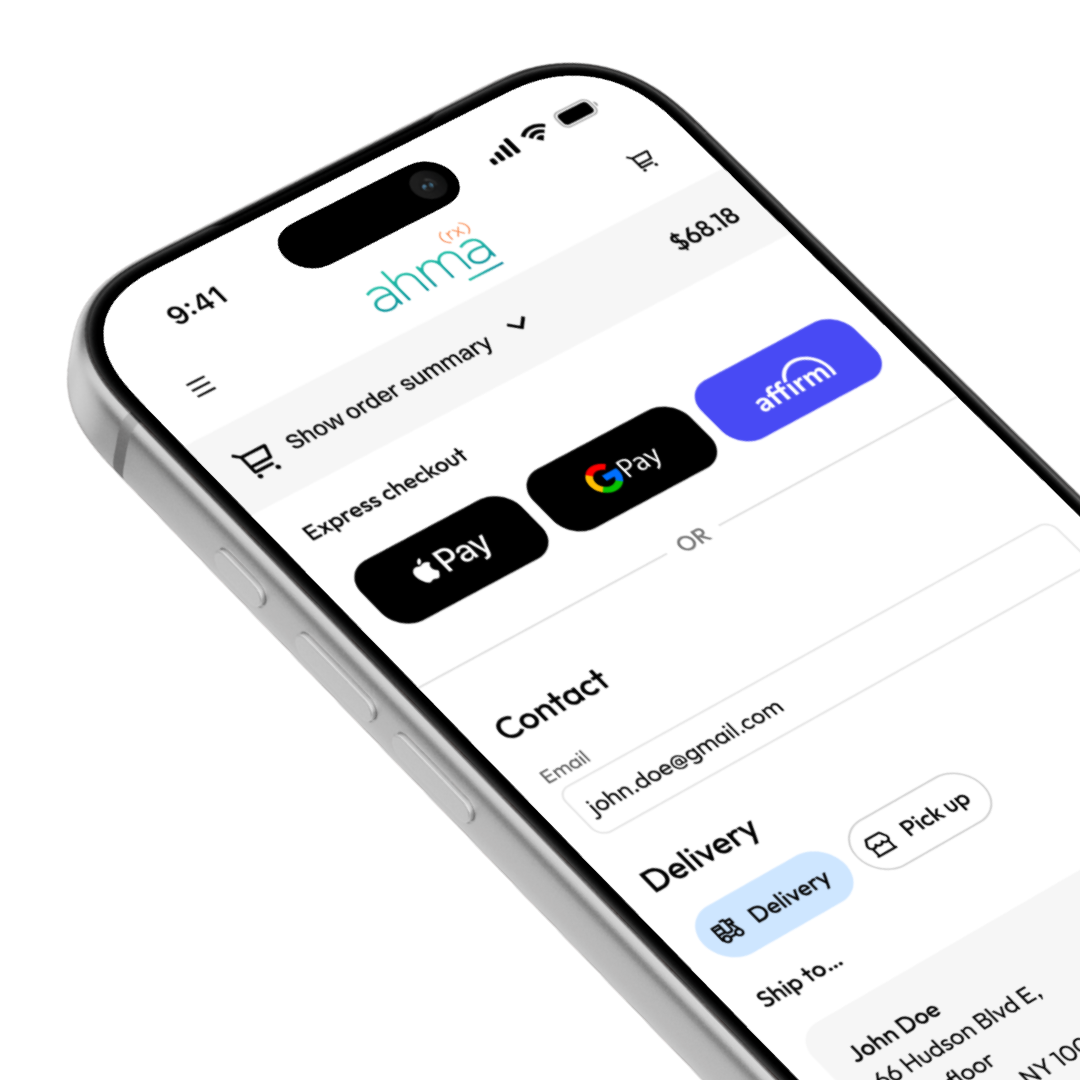

Pharmacy-native payments, embedded in your stack.
Build Tabz's pharmacy commerce layer directly into your patient experience, platform, or PMS. HIPAA BAA coverage, DEA compliance hooks, and support for HSA/FSA card payments. The core infrastructure is already there. The compliance infrastructure is already there.
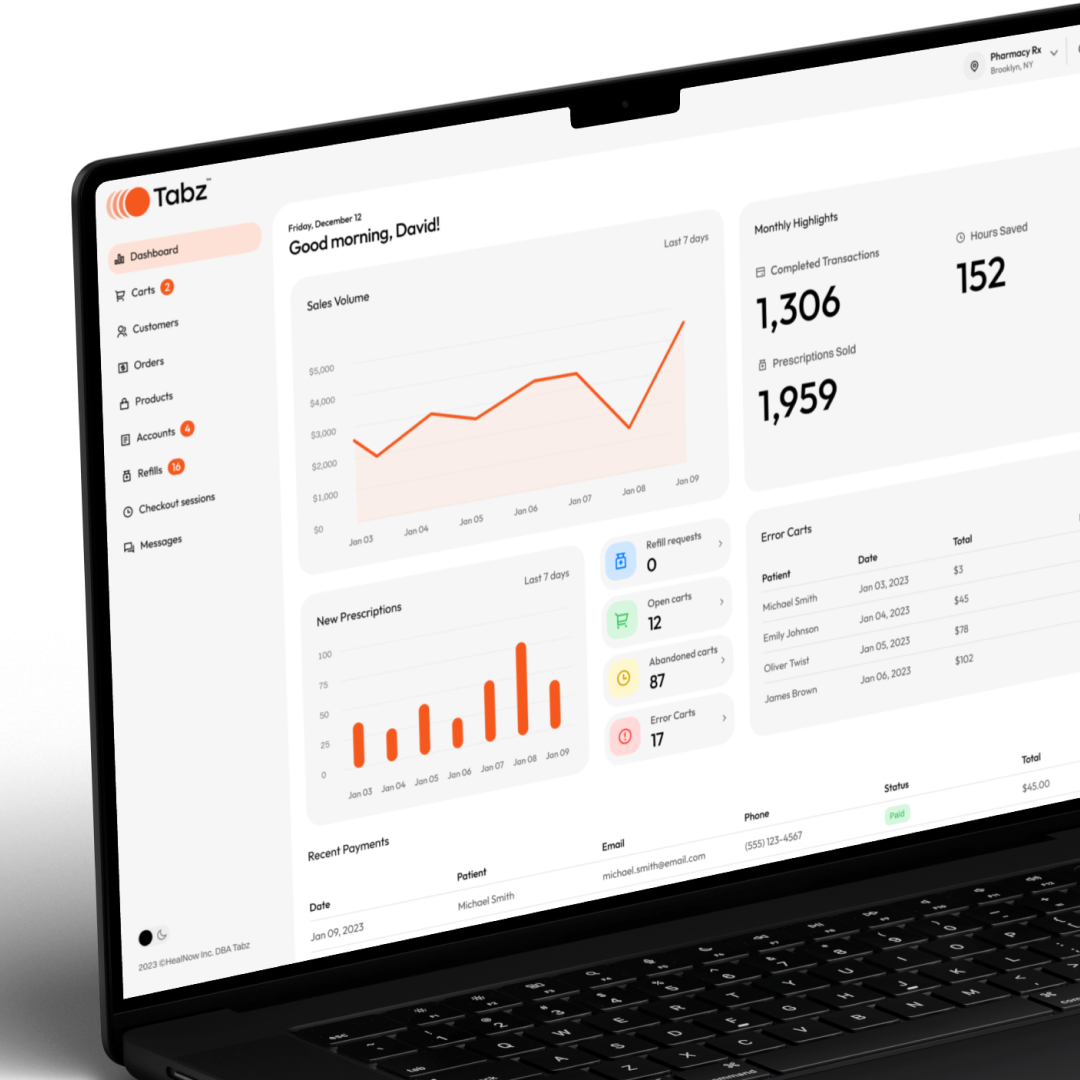

Automated updates through the workflow.
Automated text and email keeps patients informed, engaged, and paying without staff involvement. Payment links, refill reminders, RX notifications, and order updates all within your workflow.
.png)

Bill digitally. Collect faster. Eliminate paper entirely.
Send secure, branded invoices for account balances, special requests, and outstanding accounts recievable. No paper statements to print, mail, or chase. No inbound calls to process a card over the phone. Revenue moves faster, and the operational nightmare disappears.
.png)
Why specialty pharmacies need a different payment approach
Generic payment tools weren't built for the complexity of specialty dispensing. High-cost therapies, prior auth timing, and adherence requirements demand a system designed around the workflow, not bolted onto it.
High-cost medications require more payment options
A patient who can't afford a lump-sum out-of-pocket payment may abandon a therapy entirely. Flexible payment options built into the checkout flow keep patients on therapy without requiring staff to negotiate payment terms manually.
Prior authorization creates payment timing complexity
Specialty pharmacies can't always collect payment at the point of prescription. The system needs to trigger payment collection at the right moment in the workflow, not just at the point of dispensing.
Patient communication drives adherence
Specialty patients require more touchpoints than retail patients. Automated, timely communication tied to payment and fulfillment status reduces inbound calls, improves adherence, and keeps staff focused on clinical work.
Reporting at the patient level matters more in specialty
With smaller patient populations and higher per-patient revenue, specialty pharmacies need visibility into every account, not just aggregate transaction totals.
What to look for in specialty pharmacy payment software
Specialty pharmacies need a payment platform that handles the clinical and operational complexity of high-cost therapies without adding burden to staff or confusion for patients.
Flexible payment options for high-cost Rx
BNPL, ACH, HSA/FSA, and standard card should all be available at checkout so patients can afford their therapy without staff negotiating payment terms manually.
Payment links tied to prior auth status
The system should trigger payment collection at the right workflow moment — after prior auth clears — not just at the point of dispensing.
Copay assistance coordination
Patient assistance programs should apply within the checkout flow so patients see their correct responsibility without staff manually reconciling billing.
Automated patient communication
Text and email should keep specialty patients informed through prior auth, fulfillment, and delivery without requiring staff outreach at every step.
Per-patient transaction visibility
Teams should be able to track payment status, authorization stage, and outstanding balances at the individual patient level, not just in aggregate.
HIPAA-ready and PCI DSS certified
Protected health and financial data handled to the compliance standards specialty pharmacy requires — not a checkbox, built into the infrastructure.
Frequently asked questions
Tabz collects patient responsibility before dispensing, with support for Affirm BNPL and ACH alongside standard card and HSA/FSA. Patients get flexible options, pharmacies get paid before the therapy ships.
Yes. Tabz can trigger payment link delivery at specific workflow moments, including after prior auth clears, so patients are prompted to pay at exactly the right time without staff tracking it manually.
Yes. Tabz includes Affirm integration for high-cost therapies, enabling patients to split large out-of-pocket costs into manageable installments at checkout.
Automated text and email through Connect keeps patients informed on prior auth status, payment requests, fulfillment stages, and shipment updates. Fewer patients need to call in because they already have the information.
Yes. Tabz is HIPAA-ready and Level 1 PCI DSS certified, built to handle protected health and financial data at the compliance level specialty pharmacy requires.
Still have questions?
See how Tabz works for your specialty pharmacy.
Book a demo and we'll walk through how Tabz fits your dispensing workflow, your PMS, your therapy categories, and how you currently collect patient payments.
.png)
